28+ Sample Diabetes Action Plan
-

Diabetes Action Plan Template
download now -

Basic Diabetes Action Plan
download now -

Diabetes Personal Action Plan
download now -

Diabetes Goals and Action Plan
download now -

Diabetes Patient Action Plan.
download now -

Diabetes Action Plan Example
download now -

Diabetes Action Plan and Report
download now -

Diabetes National Action Plan
download now -

Diabetes Emergency Action Plan
download now -

Standard Diabetes Action Plan
download now -

Diabetes Prevention Action Plan
download now -
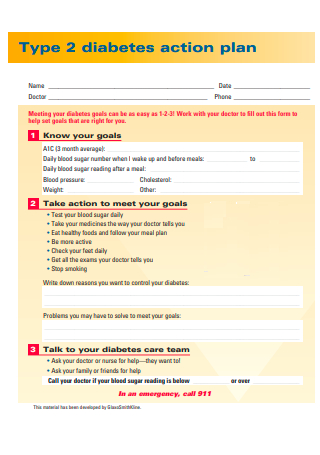
Formal Diabetes Action Plan
download now -
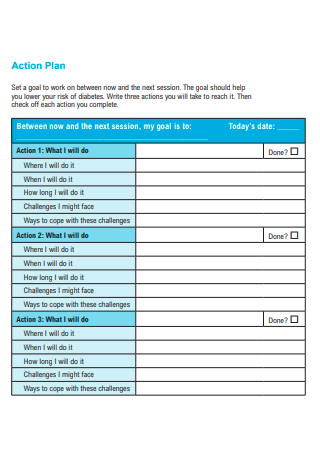
Simple Diabetes Action Plan
download now -

Diabetes Action Plan in PDF
download now -

Printable Diabetes Action Plan
download now -

Draft Diabetes Action Plan
download now -

Pediatric Diabetes Action Plan
download now -

Services Diabetes Daily Medical Action Plan
download now -

Diabetes Action Plan and Medical Alert Information
download now -
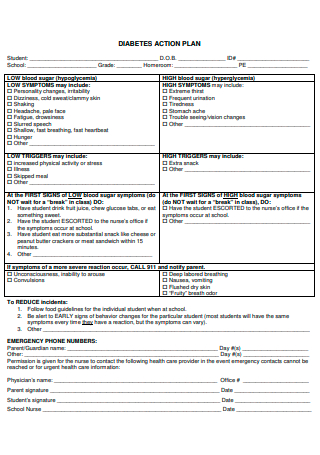

Diabetes Action Plan Format
download now -

Diabetes Smart Goals and Action Plan
download now -
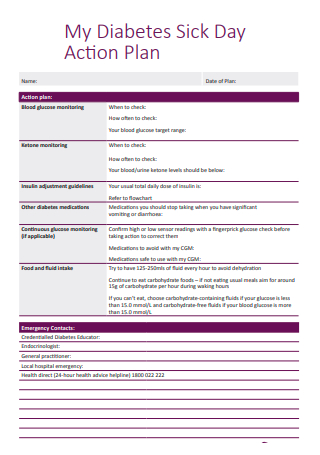

Diabetes Sick Day Action Plan
download now -

Health Services Diabetes Action Plan
download now -
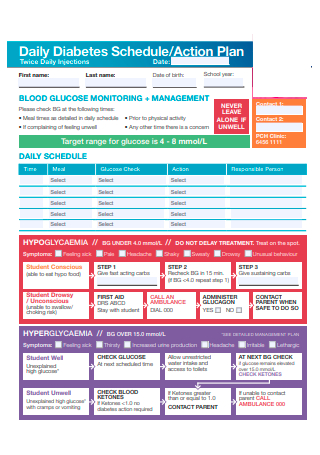

Daily Diabetes Schedule Action Plan
download now -

School Year Diabetes Action Plan
download now -

Diabetes Information Action Plan
download now -

Diabetes Action Plan Form
download now -

Student Diabetes Action Plan
download now -

Diabetes Strategy and Action Pla
download now
FREE Diabetes Action Plan s to Download
28+ Sample Diabetes Action Plan
What Is a Diabetes Action Plan?
What Is a Diabetes?
What Are the Different Types of Diabetes?
What Is the Best Way to Control Diabetes?
What Are the Steps for Treating Diabetes?
FAQs
What health problems can people with diabetes develop?
6 natural ways to prevent diabetes before it starts:
How do you manage diabetes without medication?
What are the food items to reduce sugar?
What Is a Diabetes Action Plan?
The diabetes action plan is a guide to help people manage the signs and symptoms of diabetes. You and your provider should complete this plan together at your next visit to health professionals. Moreover, the most meaningful member of a diabetes care team is you. By learning more about diabetes, creating an action plan, and sticking to that plan, you can live a healthier and more normal life.
What Is a Diabetes?
Diabetes is a disease that happens when your blood glucose or blood sugar, is too high. Blood glucose is the main source of energy and comes from the food we eat. Insulin—a hormone made by the pancreas—helps glucose from food get into the cells to be used for energy. Sometimes, the body doesn’t make enough—or any—insulin or doesn’t use insulin well. Glucose then stays in the blood and doesn’t reach the cells.
Over time, having too much glucose in the blood can cause health problems. Although diabetes has no cure, you can take steps to manage this diabetes and stay healthy.
In 2015, there are more than 1 in 4 people who didn’t know they had the disease. Diabetes affects 1 in 4 people over the age of 65. About 90-95 percent of cases in adults are type 2 diabetes.
What Are the Different Types of Diabetes?
The most common types of diabetes are type 1, type 2, and gestational diabetes.
What Is the Best Way to Control Diabetes?
Once diagnosed with diabetes, there will be some changes to your diet and lifestyle to help you manage your condition and stay healthy. Rather than trying to change everything all at once, work with your healthcare team to consider priorities and to make a diabetes care plan. Here are a few ideas to get you started:
- Exercise: Exercise and activity will help you feel better mentally, emotionally, and physically. Keep setting marks and goals for yourself to improve your fitness.
- You have more flexibility than ever before in what you eat because of the advancements in insulin. Pay attention to carbohydrates and sugars, letting yourself have the occasional treat without overindulging. Make a goal to eat more fruits and vegetables and less sodium and fat. Try to eat meals at the same time each day to keep your blood sugar levels steady.
- Medication: Talk to your provider about what medications are right for you, including insulin injections. Once your doctor has prescribed a medication, always take it as directed. When you are first diagnosed, medication may seem overwhelming. Be patient with yourself and it will become easier over time.
- Foot care: People with diabetes are more at risk for suffering from foot pain or also called peripheral neuropathy. Check your feet daily, and stem off complications by keeping them clean, dry, and moisturized.
Each person’s diabetes diagnosis is diverse, and you are the expert of yours. As you evaluate your own well-being, you will benefit from seeking the help of experienced caregivers when issues arise. These issues may comprise fever, stomach pain, extreme hunger or thirst, aches or pain, and dizziness.
What Are the Steps for Treating Diabetes?
When you have diabetes, treatment and care comes from the decisions you make on a daily basis. Directing through these daily decisions can sometimes be challenging if you don’t know where to start. Use these steps as a road map to start your journey toward well-controlled diabetes.
Step 1: Monitor the glucose
This is an essential key to good blood sugar control because it is the only way to know where you stand with your diabetes control. Fortunately, glucometers, a blood sugar machine, have come a long way. This requires a very small amount of blood and the needles are fine and hurt less when changed frequently.
Step 2: Take the medications
The medications serve a purpose in glucose control. There are various different types of medications to take for diabetes, and they work on different parts of the body. One type of medication works on the pancreas by stimulating it to excrete more insulin. Another type of medication works on fat and muscle cells to make them sensitive to the body’s own insulin.
Step 3: Be mindful of the food choices
A key part of managing diabetes is eating healthy foods every day. You want to know which foods to increase and which foods to limit. When discussing the effects of carbohydrates, protein and fat on blood sugar, carbohydrate portion control will help control blood glucose. One hundred percent of the carbohydrates you eat turn into sugar within a few hours of eating. Carbohydrates are any starch, fruit, milk, yogurt or sweet that you eat. You don’t have to avoid these foods, just be aware of the amount of it.
Step 4: Get moving
Since exercise requires energy, it helps you use up the blood sugar. Not only will exercise lower your blood sugar, it can also lower your blood pressure, decrease stress, improve circulation, improve sleep and aid in digestion. It is recommended that do 150 minutes of exercise per week to maintain a healthy weight. This equates to 30 minutes 5 times per week.
Step 5: Keep doctor’s appointments
Depending on your glucose control, you may need to see your medical doctor every six months or even every three months for checkups.
FAQs
What health problems can people with diabetes develop?
Over time, high blood glucose leads to problems such as: heart disease, stroke kidney disease, eye problems dental disease, nerve damage, and foot problems. You can take steps to lower your chances of developing these diabetes-related health problems.
6 natural ways to prevent diabetes before it starts:
Prediabetes is the phase before diabetes is diagnosed where blood sugar levels are high but not high enough to be diagnosed as diabetes. Providentially, progressing from prediabetes to diabetes is not inevitable. There are many actions you can take to reduce the risk of diabetes with these steps:
- Cut sugar and refined carbohydrates from the diet. Eating foods high in refined carbohydrates and sugar increases blood sugar and insulin levels, which leads to diabetes over time. Examples of refined carbohydrates include white bread, potatoes and many breakfast cereals. Instead, limit sugar and choose complex carbohydrates such as vegetables, oatmeal, and whole grains.
- Quit smoking if you are a smoker. Smoking can contribute to insulin resistance, which can lead to type 2 diabetes. Quitting has been shown to reduce this risk of type 2 diabetes over time.
- Watch your portions. Avoiding large portion sizes can help reduce insulin and blood sugar levels and lessen the risk of diabetes. Eating too much food at one time has been shown to cause higher blood sugar and insulin levels in people at risk of diabetes.
- Drink water. Drinking water instead of other beverages may help control blood sugar and insulin levels, reducing the risk of diabetes. Sticking with water helps you avoid beverages that are high in sugar, preservatives, and other extra ingredients.
- Eat fiber. Getting a lot of fiber is beneficial for gut health and weight management. Consuming a good fiber source at each meal can help avert spikes in blood sugar and insulin levels, which may help reduce risk of developing diabetes.
How do you manage diabetes without medication?
Instead of taking medications, try including some healthy lifestyle changes to help manage this common disease.
- Eat a healthy diet. Choose to eat more whole fruits and vegetables, more whole grains and lean proteins. Get your fats from healthy sources like avocados, nuts and olive oil. Get more high-quality proteins from eggs, beans and unsweetened yogurt. The body needs fats, carbs and proteins to function, so ensure you choose the healthiest forms. Eat whole fruits rather than drinking juice. Check food labels for hidden sugars in the ingredients list.
- Lose weight. Losing just five to 10 percent of your body weight can help control blood sugar, reduce cholesterol level and lower blood pressure. This will help reduce the risk of developing complications like heart disease and will keep you healthy.
- Exercise. Exercising 30 minutes a day can reduce blood sugar levels, decrease insulin resistance, and help regulate blood pressure and cholesterol levels. Moreover, if you can find 60 minutes per day to exercise, it can help you lose weight.
- Test your blood sugar. By testing your blood sugar regularly, you will start to see patterns. The results from certain activities lower your blood sugar. These patterns can help you plan your meals and activities so you can keep your blood sugar levels in check.
- Get enough quality sleep. Getting less than six hours of quality sleep every night can disturb the balance of insulin and blood sugar. If you are not getting good, restful sleep, try avoiding alcohol, caffeine, and spicy foods at night. You could also try lowering the temperature of your bedroom at night. Make your bedroom as dark and quiet as possible. Most importantly, establish a sleep routine by going to bed and rising at the same time every day. If these solutions don’t work, talk to your doctor about sleep apnea. Many people with Type 2 diabetes have this condition, and it can be treated with a CPAP machine at night.
- Getting regular checkups. Many difficulties of diabetes are “silent” and present no symptoms. Regular blood work to check cholesterol and kidney function will help your doctor see problems in the early stages.
What are the food items to reduce sugar?
Although factors like body weight, activity, stress, and genetics also play a role in blood sugar maintenance, following a healthy diet is essential for blood sugar control.
While some foods, including items high in added sugar and refined carbs, can contribute to blood sugar fluctuations, others can optimize blood sugar control while promoting overall health. Here are some food items to reduce sugar:
Broccoli and broccoli sprouts
Sulforaphane is a type of isothiocyanate that has blood-sugar-reducing properties. This plant chemical is produced when broccoli is chopped or chewed due to a reaction between a glucosinolate compound called glucoraphanin and the enzyme myrosinase, both of which are concentrated in broccoli.
Seafood
Seafood, counting fish and shellfish, offers a valuable source of protein, healthy fats, vitamins, minerals, and antioxidants that may help regulate blood sugar levels.
Protein is vital for blood sugar control. It helps slow digestion and prevents post-meal blood sugar spikes, as well as increases feelings of fullness. Additonally, it may help prevent overeating and promote excess body fat loss, two effects that are essential for healthy blood sugar levels.
Pumpkin and pumpkin seeds
Brightly colored and packed with fiber and antioxidants, pumpkin is a great choice for blood sugar regulation. In fact, pumpkin is used as a traditional diabetic remedy in many countries like Mexico and Iran.
Pumpkin is high in carbs called polysaccharides, which have been studied for their blood-sugar-regulating potential. Treatments with pumpkin extracts and powders have been shown to significantly decrease blood sugar levels in both human and animal studies.
Nuts and nut butter
A study has shown that eating nuts may be an effective way to help regulate blood sugar levels. Also, a review found diets emphasizing tree nuts at an average daily intake of 2 ounces (56 grams) significantly reduced fasting blood sugar and hemoglobin A1c (HbA1c), a marker of long-term blood sugar control, compared with a control diet, in people with type 2 diabetes.
Flax seeds
Flax seeds are rich in fiber and healthy fats and well-known for their health benefits. Particularly, flax seeds may help reduce blood sugar levels.
In an 8-week study in 57 people with type 2 diabetes, those who consumed 7 ounces (200 grams) of 2.5% fat yogurt containing 1 ounce (30 grams) of flax seeds per day experienced substantial reductions in HbA1c, compared with those who consumed plain yogurt.
Many things can cause your blood sugar to fall riskily low (hypoglycemia), including taking too much insulin, missing or delaying a meal, not eating enough food for the amount of insulin you’ve taken, exercising very energetically, and drinking alcohol, especially on an empty stomach. After having diabetes for several years, many people develop hypoglycemia unawareness— they lose the ability to detect the onset of hypoglycemia. Risk factors include frequent hypoglycemia, nerve damage, and intensive insulin therapy.
For this reason, it is vital to involve others in your emergency plans. Train family members, coworkers, and friends to spot the signs of hypoglycemia, especially moderate to severe symptoms, because you may not be able to ask for help in an emergency. Take care of your health and always know what you need to plan out for your diet.
